Keratoconus
Laser vision correction and Keratoconus
Although keratoconus is not an absolute contraindication for laser vision correction, the majority of eye clinics worldwide would refuse a laser procedure to such patients. The reason is the much higher risk – there is a possibility that the treated keratoconus patients would need spectacles and/or contact lenses in the future.
Laser procedures in keratoconus patients are usually performed with a planned corneal crosslinking in order to strengthen the cornea and minimize the risks. Eye hospital "Luxor" recommends to all the patients with a history of keratoconus NOT to undergo laser vision correction.

What is keratoconus?
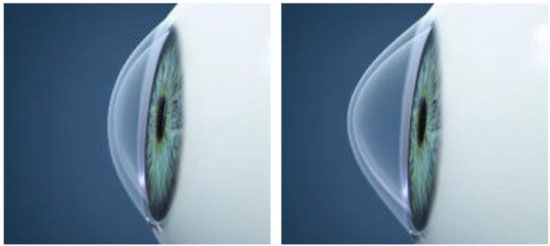
The cornea is the strongest optical element of the eye. The light refracts through it and then through the lens, and the image is projected onto the retina. The normal surface of the cornea is smooth and shiny, with a slightly more protruding center than at the edges.
In patients with keratoconus, the cornea progressively protrudes and thins at a certain lace by acquiring an irregular cone-like shape. Even the smallest changes in its shape lead to deterioration in vision. An irregular corneal astigmatism appears, which is difficult (sometimes impossible) to correct with glasses or contact lenses. In principle, both eyes are affected, but to varying degree.
The causes of the disease have not yet been fully studied, but are most likely genetic. In the initial stage of development of keratoconus (usually in young age), mild manifestations of astigmatism and nearsightedness can occur, which can be corrected with glasses or contact lenses, as they are periodically adjusted. However, with the progress of the disease, this proves to be insufficient to compensate the disease, and then it is necessary to wear hard contact lenses or special contact lenses for keratoconus.
Complaints and symptoms
- Blurred vision
- Often necessity of diopter adjustment
- Progression of astigmatism
- Progression of nearsightedness
Diagnostics of keratoconus
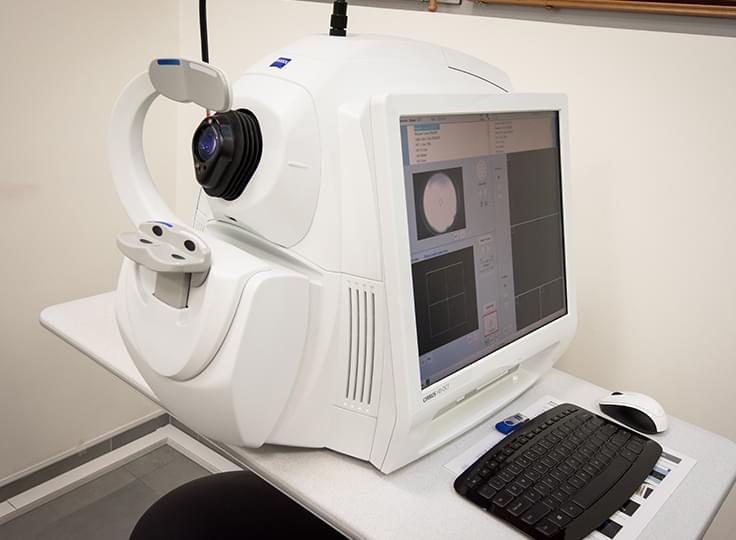
In Eye Hospital Luxor, keratoconus is diagnosed with the most advanced technology. The most accurate diagnosis of the disease is done with the so-called corneal topographers - Placido disks based as Atlas of Carl Zeiss or Scheipflug based as Pentacam of Oculus, which maps the characteristic changes in anterior and posterior corneal curvature. The corneal thinning in keratoconus can be determined extremely accurately by means of pachymetry mapping with the optical coherence tomographs Cirrus 6000 and Cirrus 5000 (Carl Zeiss). Biomechanical corneal changes (weakening) in keratoconus can be detected and followed-up with the device Corvis (Oculus).
Atlas, Pentacam and Corvis

Cirrus 6000 and Cirrus 5000
Treatment of keratoconus
The latest method for treatment patients with keratoconus is the corneal cross-linking procedure (CXL), which strengthens the cornea – it is irradiated with ultraviolet light in the presence of Riboflavin (vitamin B2). This stimulates the formation of new collagen connections. The goal is to stop the progressive increase in diopters. The vision does not improve after the procedure. It is possible that some of the diopters of the keratoconus patients are removed if the crosslinking is combined with a laser vision correction (at the discretion of the physician).
Another option for adjustment of the refractive power of the eyes with a keratoconus is to place the so-called kerathorins in the cornea. These are implants from artificial, biocompatible substance that flatten the conical shape of the cornea, make it more correct and thus improve the vision.
In the final stages of keratoconus, when the vision is significantly reduced (about 15% of cases), corneal grafting (keratoplasty), may be necessary.
LightLink CXL Corneal Cross-Linking System
Eye Hospital Luxor is equipped with LightLink CXL Corneal Cross-Linking System a state-of-the-art system for crosslinking procedures.
It is manufactured by the American company LightMed, which is world famous for the high quality of its products in the field of ophthalmology.
Main technical advantages:
- 1-30mJ Ultra Efficient UVA system with optical homogenizer
- built-in Standard & Rapid crosslink protocols
- pulsed Cross Linking Function
- procedure Customization functions